Just as our physical strength decreases with age, our eyes also exhibit an age-related decline in performance. Some age-related eye changes, like presbyopia, are normal and aren’t a sign of disease. However, many eye diseases often surface as we age. Understanding the most common conditions, their causes, and potential treatments is essential to preserve your eyesight.
Several disorders can affect the retina – a layer of cells at the back of your eye that are sensitive to light. Let’s delve into these retinal disorders so you’re better prepared and informed.
Age-Related Macular Degeneration
Age-related macular degeneration (AMD) is one of the most common retinal disorders among older adults. It’s a disease that blurs the sharp, central vision needed for activities like reading and driving. AMD is classified into two types:
- Dry AMD: This form is more common and less severe, characterized by the thinning of the macula, the part of the retina responsible for sharp central vision.
- Wet AMD: Less common but more serious, this condition type involves the growth of abnormal blood vessels underneath the retina, leading to leakage of fluid and blood.
Symptoms of Age-related Macular Degeneration (AMD):
Age-related Macular Degeneration primarily affects the central part of your vision. The disease comes with specific symptoms, including:
- Blurriness or dark areas in the center of vision
- Straight lines appearing as wavy or distorted
- Difficulty in adapting to low light levels
- Decreased brightness of colors
Diabetic Retinopathy
Another common retinal disorder is Diabetic Retinopathy, which affects individuals with diabetes. High blood sugar levels can damage the blood vessels in the retina, leading to vision problems.
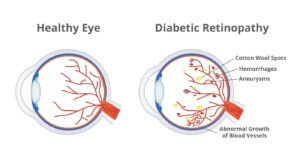
There are two stages of Diabetic Retinopathy:
People with diabetes can sometimes face eye problems due to high blood sugar. This is known as Diabetic Retinopathy, and it usually comes in two parts:
- Early stage or Non-proliferative Diabetic Retinopathy (NPDR): During this first stage, the blood vessels in your eye’s retina (the back part of the eye that catches light) weaken because of too much sugar in your blood. This weakness causes small bumps called microaneurysms that can leak blood and other fluids into the retina. This can make the retina swell and affect your vision. You might not notice any changes to your sight during this stage, but regular eye check-ups can catch these issues early before they worsen.
- Advanced stage or Proliferative Diabetic Retinopathy (PDR): This is when things get more serious. Because of all the damage to your eye’s blood vessels, your retina starts to grow new ones to try and fix the problem. But these new blood vessels are weak and can easily bleed. This bleeding can cloud the inside of your eye and cause serious vision problems. Sometimes, these new blood vessels can also create scar tissue that can pull the retina away from the back of the eye, leading to another problem called retinal detachment.
Symptoms of Diabetic Retinopathy
Diabetic Retinopathy is a condition that affects people with diabetes. High blood sugar levels can damage the blood vessels in the retina, leading to the following symptoms:
- Seeing floaters (specks or lines floating in your field of vision)
- Blurred vision
- Fluctuating vision
- Sudden vision loss
- Dark or empty areas in vision
- Difficulty with color perception
Retinal Detachment
Retinal detachment is a serious eye condition that can lead to loss of sight if not treated promptly. It happens when the retina (the part of your eye that senses light and sends images to your brain) pulls away from the back of the eye. This condition comes in three forms, each with its cause:
- Rhegmatogenous Retinal Detachment: This is the most common type and happens when a hole or tear in the retina lets some of the gel-like substance that fills the eye (vitreous fluid) pass through. This fluid then collects under the retina, causing it to peel away from the back of the eye. Think of it like wallpaper peeling off a wall. This type can cause a sudden change in vision, like seeing lots of ‘floaters’ or light flashes or feeling like a curtain has been pulled over your field of view.
- Tractional Retinal Detachment: This type happens when scar tissue on the retina’s surface shrinks and pulls the retina away from the back of the eye. This type is often seen in people who have uncontrolled diabetes, which can cause abnormal blood vessels to grow on the retina and lead to scar tissue formation.
- Exudative Retinal Detachment: This type is a bit different. Here, there are no holes or tears in the retina. Instead, fluid leaks from blood vessels underneath the retina and collects under it, causing it to lift away from the back of the eye. This often happens because of eye conditions like inflammation or age-related macular degeneration.
Symptoms of Retinal Detachment
Retinal detachment is a serious condition where the retina pulls away from its normal position. Symptoms of this disorder can be sudden and include:
- The sudden appearance of many floaters (specks drifting through your field of vision)
- Seeing flashes of light in one or both eyes
- Reduced peripheral (side) vision
Retinal Vein Occlusion
Retinal Vein Occlusion (RVO) occurs when the tiny veins that carry blood away from the retina, the light-sensitive layer at the back of the eye, get blocked. This blockage can cause blood and other fluids to accumulate in the retina, leading to swelling and damage that affects your vision.
Retinal Vein Occlusion typically comes in two forms:
- Branch Retinal Vein Occlusion (BRVO): This is the milder form of RVO. In this condition, only a tiny portion of your retina’s veins gets blocked, usually at a place where your artery has crossed over it. While it may cause some vision loss or distortion, its impact is usually not as severe as the other form of RVO.
- Central Retinal Vein Occlusion (CRVO): This is the more severe form of RVO. In CRVO, the main vein that carries blood away from your retina becomes blocked, causing a significant impact on your vision. This form of RVO can lead to severe vision loss and may even cause blindness in the affected eye.
Symptoms of Retinal Vein Occlusion
Retinal Vein Occlusion is a condition that can lead to severe vision problems if not promptly treated. Recognizing the symptoms early can significantly improve the chances of successful treatment. The common signs of this disorder include:
- Sudden blurring or loss of vision, usually in one eye
- Seeing floaters, which are tiny dark spots or lines floating in your field of vision
- Having a blind spot in your field of vision
- Seeing the distorted or reduced vision, especially in one part of the visual field
Preventing Age-Related Retinal Disorders
Age-related retinal disorders can significantly impact vision, but there are steps you can take to reduce the risk of developing these conditions. Here are some preventive measures:
Regular Eye Exams: Annual eye check-ups can catch early signs of retinal disorders, leading to earlier treatment and a better outcome.
- Regular comprehensive eye exams
- Tests for glaucoma
- Retinal screening for people with diabetes
Healthy Lifestyle Choices: A balanced diet and regular exercise can help manage conditions that increase the risk of retinal disorders.
- Eating a diet rich in fruits, vegetables, and fish
- Regular exercise to maintain healthy body weight
- Avoiding smoking
- Limiting alcohol consumption
Manage Underlying Conditions: If you have a chronic condition such as diabetes or hypertension, it’s essential to manage it effectively.
- Regularly monitoring blood sugar levels if you have diabetes
- Keeping blood pressure and cholesterol levels in check
- Taking prescribed medications as directed
Protect Your Eyes: Protect your eyes from harmful ultraviolet (UV) light and potential injury.
- Wearing sunglasses that block UV rays
- Using protective eyewear during sports or activities could lead to an eye injury.
Contact Us
Implementing these steps into your daily routine can protect your eyes and potentially prevent age-related retinal disorders. Remember, your eye health is an integral part of your overall well-being, and taking preventive measures now can significantly benefit your vision in the long run.
If you have been experiencing vision problems, please do not hesitate to find help. Schedule your appointment with Florida Eye today!