Corneal Dystrophies
Corneal dystrophies describe a number of eye conditions caused by abnormal cellular function and development. When these substances accumulate too greatly, light cannot be focused properly, which affects images being processed by the brain. Most corneal dystrophies are inherited and involve both eyes. Some patients experience no symptoms at all, while others face extensive vision loss, pain, light sensitivity or a scratchy feeling as if a particle is in the eye.
There are more than 20 different types of corneal dystrophies. Some of the most common ones are Fuchs’ dystrophy, keratoconus, and lattice dystrophy. The majority of corneal dystrophies progress slowly, starting in one layer of the cornea and sometimes advancing to other layers over time.
Treatment of corneal dystrophies will depend on the condition diagnosed and the severity of its symptoms. In many cases, conservative measures will be initially used, such as wearing special contact lenses that can protect the cornea. For some patients with corneal dystrophies, a corneal transplant may eventually become necessary to restore vision.
Keratoconus
A progressive eye disease in which the normally round cornea thins and begins to bulge into a cone-like shape. This cone shape deflects light and can cause distorted vision.
Early stages of keratoconus can be treated with eyeglasses or soft contact lenses. For more advanced cases, rigid gas-permeable contact lenses and scleral lenses must be used for optimal vision. For patients with progressive keratoconus, a treatment called ‘collagen cross-linking’ is recommended to halt the progression. This treatment is also done for patients with post-LASIK ectasia, a similar progressive condition of the cornea. If keratoconus persists with deep central scarring, corneal transplant surgery can be performed to correct the condition.
Appointment Request
SURGICAL TREATMENTS
A cornea transplant replaces diseased or scarred corneal tissue with healthy tissue from an organ donor. A graft replaces central corneal tissue (damaged due to disease or eye injury) with healthy corneal tissue donated from a local eye bank. Corneal transplants we perform:
- Descemet membrane endothelial keratoplasty (DMEK)
- Descemet stripping endothelial keratoplasty (DSEK)
- Penetrating keratoplasty (PK)
- Deep anterior lamellar keratoplasty (DALK)
- Artificial Cornea (Keratoprosthesis)
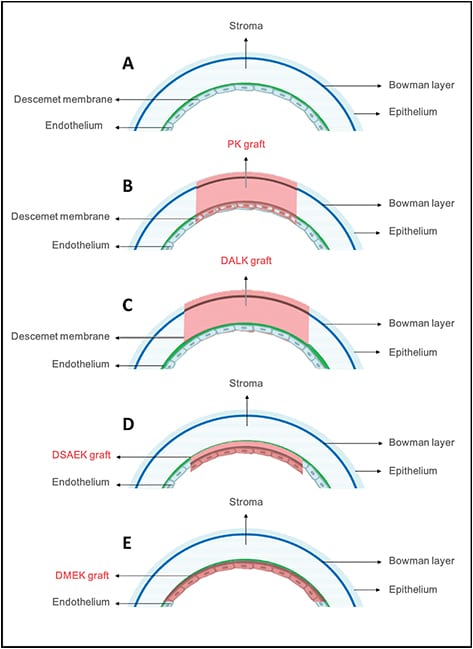
As shown in the corneal tissue graft figure, the different types of transplants remove and replace different parts of the cornea. Your doctor will suggest the most appropriate type of transplant for you depending on your corneal disease.
DSEK versus DMEK: Both surgical techniques are utilized for the treatment of endothelial corneal dystrophies, such as Fuch’s endothelial dystrophy. What’s the difference?
- DMEK has BETTER visual outcomes (approximately 20/25 versus 20/40 on average after DSEK)
- Faster visual recovery with DMEK
- Lower risk of rejection
- Patients prefer final outcome of DMEK, even though longer positioning time is required
- However, not all patients are good candidates for DMEK. Your surgeon will discuss the best option for you.
Penetrating Keratoplasty (PK): For full thickness corneal diseases, keratoconus with deep scarring, severe bullous keratopathy
Deep Anterior Lamellar Keratoplasty (DALK): Keratoconus, stromal dystrophies, superficial corneal scarring
Artificial Cornea (Keratoprosthesis): This procedure is often recommended after multiple standard corneal transplants have failed or when such a transplant would be unlikely to succeed. Thus keratoprosthesis implantation is a procedure designed to help patients whose conditions are the most difficult to treat.